
Embark on an enlightening journey through the stages of labor and delivery, as we guide you from the first contraction to holding your baby in your arms. This comprehensive guide is here to ensure you are prepared and confident for the miraculous journey of childbirth and to make you well-equipped for this life-changing experience.
Introduction to Labor and Delivery
Labor and delivery represent a significant phase in a woman’s life and mark the beautiful culmination of pregnancy. The process of labor and birth is usually divided into three stages that define how labor progresses, starting from the onset of true labor contractions to the birth of your baby and finally, the delivery of the placenta. Each stage has its unique signs, length of labor, and expectations. Understanding the normal flow of these stages can help demystify the process, making the experience less daunting and more empowering.
Labor usually begins spontaneously, but in some instances, labor induction might be necessary. As the estimated date of delivery approaches, you might find yourself constantly on the lookout for the telltale signs of labor. The start of labor is different for every woman and every pregnancy. It’s important to understand the sign and stages of labor to ensure you’re well-prepared when you go into labor.
The first stage of labor, also known as the beginning of labor, is the longest and involves the effacement (thinning out) and dilation (opening up) of the cervix. This stage is subdivided into early labor, active labor, and transition phase. The second stage of labor involves the delivery of your baby, and the third stage involves the delivery of the placenta.
It’s worth noting that, while the description of labor stages can seem linear, labor occurs in a spectrum. The progression of labor is influenced by many factors, and sometimes, it may not follow the ‘textbook’ sequence. Thus, while this guide aims to present a comprehensive picture of normal labor and delivery, variations can and do happen.
In the following sections, we’ll delve deeper into the stages of labor and delivery, starting with the signs of labor that hint your baby is ready to make their grand entrance.
Note: Each labor experience is unique and can deviate from the norm. Always consult your healthcare provider for advice tailored to your specific circumstances.
Signs of Labor: How to Recognize the Real Deal?

As you approach your estimated date of delivery, anticipation builds up, and every twinge might make you wonder if labor has started. It is crucial to differentiate between true labor and false labor, often called Braxton Hicks contractions. Recognizing the signs of labor is the first step in preparing for the birth of your baby.
What are Braxton Hicks Contractions?
Braxton Hicks contractions, also known as “practice contractions” or “false labor,” can begin as early as the second trimester. These contractions are the uterus’s way of preparing for labor and delivery, but they do not signify the onset of labor. They are typically irregular, infrequent, and do not increase in intensity or frequency over time.
Signs of True Labor
True labor contractions have a distinct pattern. They start irregularly but soon develop a regular pattern, growing stronger, longer, and closer together. Unlike Braxton Hicks contractions, true labor contractions do not stop when you move or change positions. These are some of the signs that labor may be starting:
1. Contractions
In true labor, contractions become regular, stronger, and more frequent over time. Each contraction usually lasts about 30-70 seconds, giving rise to an intense period of discomfort or pain in your lower back and abdominal area.
2. Changes in Cervix
As labor begins, the cervix starts to dilate and efface (thin out). This is often accompanied by a “bloody show,” a small amount of blood mixed with mucus, which is a normal sign of labor.
3. Water Breaking
Also known as the rupture of membranes, this can occur at any time during labor, or before labor begins. It can feel like a sudden gush of water or a steady trickle. If you suspect your water has broken, contact your doctor immediately.
Remember, every woman’s experience with labor is unique. Some women may experience all the signs, while others may not. Some women go into labor within hours or days after experiencing these signs, while others may take longer. If you think you’re in labor, it’s always a good idea to call your doctor or go to the hospital.
Up next, we’ll delve deeper into the stages of labor and delivery, starting with the first stage of labor: the early labor, active labor, and transition phase. Understanding these phases will provide you with the necessary insights to better handle labor when it occurs.
The First Stage of Labor: What to Expect?
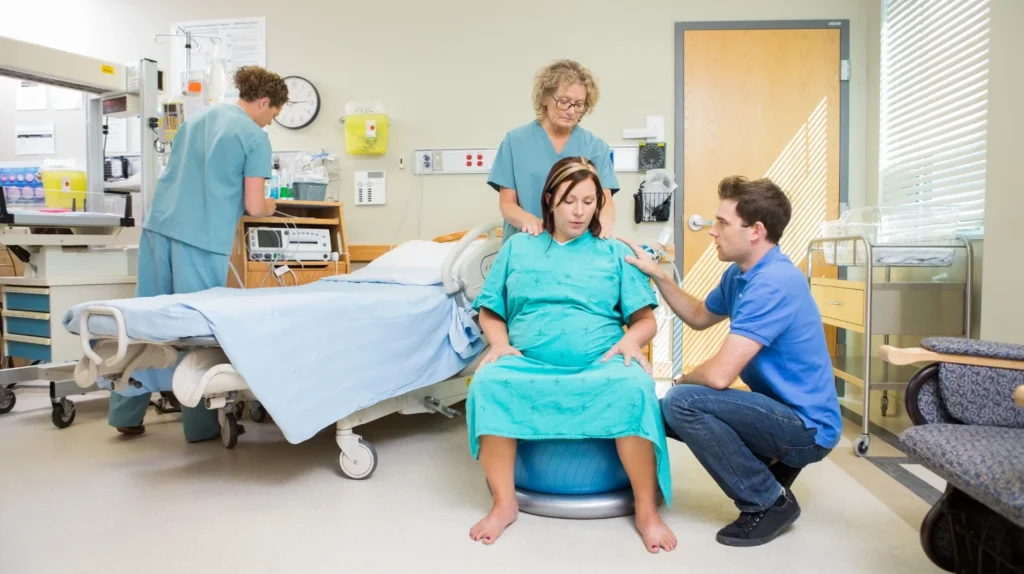
The first stage of labor is the longest and involves three phases: early labor, active labor, and the transition phase. Each phase plays a crucial role in the process of labor and delivery, preparing both the mother’s body and the baby for birth. Understanding these phases can help you recognize the progress of your labor and know when it’s time to go to the hospital.
Early Labor: The Onset of the Journey
Early labor, the least intense phase of labor, is the beginning of the labor process. The signs of early labor are typically mild and may last a few hours to a few days. During this phase, contractions become regular and increase in intensity and frequency. However, they may still be relatively far apart, often five to twenty minutes apart and lasting about 30 to 45 seconds each.
Women in early labor may experience lower back pain, cramping, and changes in vaginal discharge. This phase ends when the cervix is about 3 to 4 centimeters dilated.
For many women, early labor is manageable. You may be able to relax, take short walks, or even rest. It’s essential to stay hydrated and nourished during this phase, as you’ll need the energy for the more intense stages of labor to come.
Active Labor: When Things Get Real
Once the cervix dilates to about 4 to 7 centimeters, active labor begins. This phase is more intense and generally lasts around 3 to 5 hours. The contractions during active labor are longer, stronger, and closer together, usually three to five minutes apart and lasting about 45 to 60 seconds each.
During active labor, your doctor may monitor your progress and the baby’s heart rate more closely. Pain management, such as epidural analgesia, may be discussed during this phase if not already administered.
It’s essential to maintain focus and use your breathing exercises during contractions. Consider changing positions to help manage labor pain.
Transition Phase: The Final Hurdle of the First Stage
The transition phase is the final and the most challenging part of the first stage of labor. It begins when the cervix is about 8 centimeters dilated and ends when it’s fully dilated to 10 centimeters, ready for the baby’s delivery.
Contractions during the transition phase are very intense, usually lasting about 60 to 90 seconds with only a 30-second to 2-minute rest in between. You might feel pressure in the lower back and rectal area, which is a sign that the baby is moving into the birth canal.
Due to the intensity of contractions, some women may experience nausea, hot flashes, or chills. This is completely normal, and it’s important to have the right support and pain relief measures in place.
Once the transition phase ends, the first stage of labor is over, and the second stage – the delivery of your baby – begins. It’s crucial to keep communication open with your doctor throughout your labor to ensure safe and successful delivery.
The Second Stage of Labor: The Arrival of Your Baby

The second stage of labor, often referred to as the “pushing stage,” begins when the cervix is fully dilated at 10 centimeters and ends with the birth of your baby. This is the moment you’ve been waiting for – the arrival of your newborn.
Contractions during the second stage of labor continue to be strong but may spread out, allowing for brief periods of rest. These contractions help push your baby down the birth canal. During this stage, your healthcare provider will guide you on when to push with the contractions to help move your baby down the birth canal.
You might find relief in changing positions during this stage; this can help you stay comfortable and assist in the baby’s descent. Options could include squatting, lying on your side, or being on all fours.
As your baby descends, you may experience an intense urge to push, often described as feeling similar to the need to have a bowel movement. It’s crucial to follow your body’s cues and the guidance of your doctor. Pushing before you’re fully dilated or when not instructed to do so could lead to exhaustion or complications.
Once your baby’s head is visible in the birth canal – a moment known as “crowning” – you are close to giving birth. At this point, your healthcare provider may instruct you to push more gently or to stop pushing altogether to prevent tearing.
When your baby is fully out, the second stage of labor ends. This stage’s length can vary greatly from one woman to another, lasting anywhere from a few minutes to several hours, especially for first-time mothers.
The arrival of your baby is an incredible moment filled with a range of emotions. After your baby is born, they will be placed on your chest for immediate skin-to-skin contact to promote bonding and help regulate the baby’s body temperature.
The labor process, however, is not quite finished yet. Following the birth of your baby comes the third and final stage of labor: the delivery of the placenta.
The Third Stage of Labor: Delivery of the Placenta

The third stage of labor is the shortest and final stage of labor, commencing after the birth of your baby and ending with the delivery of the placenta. Although the birth of your baby signifies the climax of labor and delivery, the process isn’t quite complete until the placenta has been delivered.
The placenta, also known as the “afterbirth,” is the organ that has nourished your baby throughout your pregnancy. It’s attached to the inside of your uterus and connected to your baby by the umbilical cord. Once your baby has been born, your uterus will continue to contract, these contractions now serving to detach and expel the placenta.
Usually, within 5 to 30 minutes after your baby’s birth, you’ll experience another set of contractions, though these are typically less painful than labor contractions. Your healthcare provider may ask you to push one more time to help deliver the placenta. They may also gently tug on the umbilical cord to encourage its release.
Once the placenta is delivered, your doctor will inspect it to ensure it’s intact. Any remaining fragments inside the uterus can cause complications like excessive bleeding.
This stage is also when any tearing or episiotomies (a surgical cut made at the opening of the vagina to aid delivery) will be stitched and repaired. Your healthcare provider will monitor you for signs of excessive bleeding or other complications.
Although the delivery of the placenta marks the end of labor and delivery, your care team will continue to monitor you and your baby in the hours following birth to ensure both of you are transitioning well into the postpartum period.
Labor and delivery is a unique and personal journey for every woman. Understanding the stages of labor can help you prepare for the experience, making it feel less overwhelming and more empowering.
Types of Delivery: Normal and Cesarean
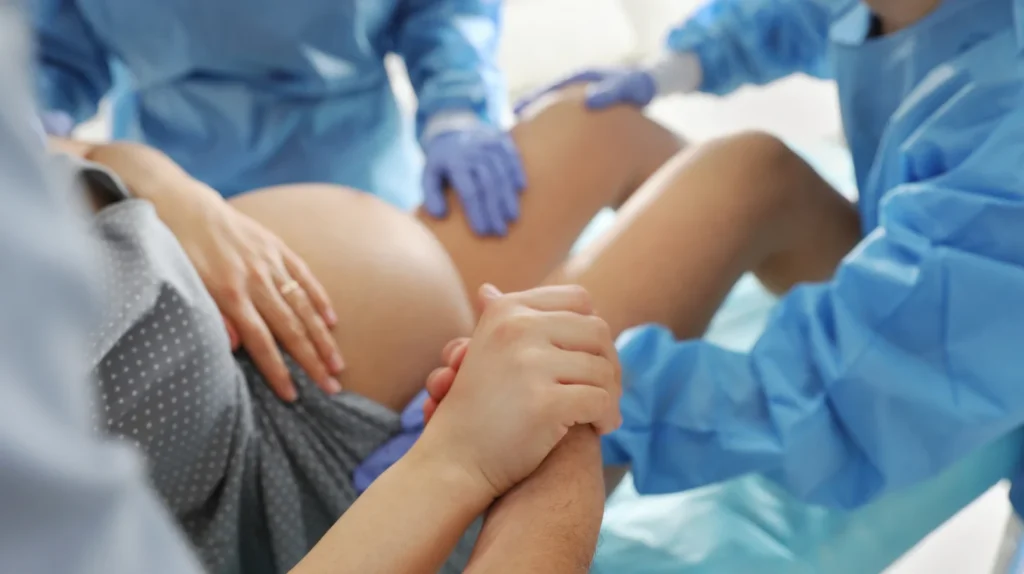
When it comes to the delivery of your baby, there are two primary types: vaginal (normal) delivery and cesarean delivery. The progression of your labor and the condition of your baby will significantly determine the type of delivery you’ll have.
- Normal Delivery: Also known as vaginal delivery, this is the most common and traditional type of childbirth. It involves three main stages of labor: the dilation of the cervix, the birth of your baby, and the delivery of the placenta. During a vaginal delivery, you’ll actively participate by pushing your baby through the birth canal.
There are also sub-types of normal delivery, including spontaneous vaginal delivery (where labor starts on its own without any medical intervention), assisted vaginal delivery (forceps or vacuum extraction is used to help guide the baby out of the birth canal), and induced labor (medications or other methods are used to initiate labor).
- Cesarean Delivery: A cesarean delivery, or C-section, is a surgical method of birth where the baby is delivered through an incision in the mother’s abdomen and uterus. Cesarean deliveries are typically performed when a vaginal delivery would put the baby or mother at risk. Some reasons for a cesarean delivery include multiple births (twins, triplets, etc.), a large baby, breech position, certain medical conditions in the mother, or the baby showing signs of distress.
The choice between a vaginal delivery and a cesarean delivery is usually determined by the doctor based on the health of the mother, the baby’s positioning, and any potential complications. It’s crucial to discuss your birth plan and any questions or concerns you may have about the type of delivery with your doctor provider before your estimated date of delivery.
Regardless of the mode of delivery, the ultimate goal is always the same: to ensure the safety and health of both mother and baby during the labor and birth process.
Managing Labor Pain: What are Your Options?

Labor can be an intense experience and managing labor pain is an important part of the process. Every woman’s labor is unique, including the type, intensity, and location of pain she may experience. Thankfully, there are several options available to manage labor pain, and you can discuss these with your doctor to create a personalized plan that suits your needs and wishes.
- Natural Pain Relief: Some women choose to manage labor pain using natural methods. These can include deep breathing techniques, visualization, yoga, meditation, massage, and changing positions frequently. The support of a loved one can also be beneficial.
- Medication-Based Pain Relief: There are several types of medication available to help manage labor pain. Analgesics can lessen the pain without causing a total loss of feeling. These can be administered through an IV or an injection. Another commonly used medication-based method is epidural anesthesia, which provides numbness from the waist down. Your mobility might be limited with an epidural, but most women can still push effectively when it’s time for delivery.
- Pain Medication through Inhalation: Some hospitals offer nitrous oxide (laughing gas) as an option for managing labor pain. This option allows you to control the amount of gas you’re inhaling, and it can be used at any stage of labor.
Remember, your pain management plan can always be adjusted during labor as necessary. What’s most important is your comfort, safety, and the well-being of your baby. It’s beneficial to discuss your pain relief options well before your estimated date of delivery, allowing time to consider your choices and make an informed decision.
The process of labor and delivery, although physically and emotionally intense, ends with the extraordinary reward of your baby’s birth. Understanding your options for managing labor pain will help you feel more prepared and in control during this transformative event.
Inducing Labor: When and Why is it Needed?

Labor induction is the process of using medications or other methods to start (induce) labor. It is a common procedure, but it’s not always necessary – labor usually starts on its own. However, in certain situations, it can be beneficial and even lifesaving for both mother and baby. Here’s what you need to know about labor induction.
- When is Labor Induced?
Labor may be induced for various reasons. Here are some common situations:
- Post-Term Pregnancy: If you’re two weeks or more past your due date, induction of labor might be recommended. Extended pregnancies can cause problems for both you and your baby.
- Rupture of Membranes: If your water breaks (rupture of membranes) but labor does not begin, induction of labor may be necessary to avoid an infection.
- Medical Conditions: Certain medical conditions, such as high blood pressure, preeclampsia, diabetes, or heart disease, can make it dangerous to continue the pregnancy.
- Fetal Growth Restriction: If the doctor is concerned about your baby’s growth in the womb, labor might be induced.
- Decreased Fetal Activity: Reduced movement of your baby could indicate potential problems with the placenta or umbilical cord. In such cases, labor may be induced.
- How is Labor Induced?
Several methods are used for labor induction:
- Medications: Drugs like Syntocinon (a synthetic form of the hormone oxytocin) can be used to stimulate contractions.
- Ripening the Cervix: Prostaglandins (hormones) can be used to prepare (ripen) the cervix for labor.
- Stripping the Membranes: This procedure involves the healthcare provider sweeping their finger over the thin membranes that connect the amniotic sac to the wall of the uterus.
- Breaking Water (Amniotomy): The doctor may make a small opening in the amniotic sac to induce labor. This is often done during active labor and can make contractions more effective.
It’s important to remember that the decision to induce labor should be made in consultation with your doctor and be based on the best interest of both mother and baby. The goal is always a safe delivery and a healthy baby.
KEY TAKEAWAYS
1. Labor and delivery are divided into three stages: early labor, active labor, and transition (first stage); birth of the baby (second stage); and delivery of the placenta (third stage).
2. It’s important to distinguish between Braxton Hicks (false labor) and true labor contractions to know when labor has begun.
3. Various options for managing labor pain are available, ranging from natural techniques to medical interventions like epidurals.
4. Both vaginal and cesarean deliveries are common, with the type of delivery often determined by the health and safety of the mother and baby.
5. Induction of labor may be necessary under certain circumstances where waiting for spontaneous labor carries risks.
Conclusion: Embracing the Labor and Birth Experience
Labor and delivery constitute a profound and transformative journey. While it is a highly individualized experience that can be unpredictable, understanding the stages of labor, recognizing signs of true labor, and being aware of your options for pain relief and types of delivery can equip you to better navigate this extraordinary event.
From the onset of labor to the delivery of your baby and the placenta, each stage moves you closer to the moment you’ve been waiting for – the birth of your baby. Every birth story is unique, and all lead to the same beautiful outcome: the arrival of your baby.
At the end of this journey, no matter how labor and delivery unfold, it ends with the miraculous birth of your baby. Embrace the journey, trust your body, and remember, you are stronger than you think. You’re about to embark on a whole new journey of parenthood, filled with its own challenges, joys, and rewards. Welcome to this new stage of your life.
If you found this article helpful, please share it with your friends on WhatsApp, Facebook, or Twitter using the buttons above or below the article.
Frequently Asked Questions (FAQs)
What is the definition of labor?
Labor is the set of processes that lead to the delivery of the fetus and the expulsion of the placenta from the woman’s body.
What are the different stages of labor?
The three stages of labor are the early phase, active phase, and the transition phase.
When does labor typically begin?
Labor usually begins between 37 and 42 weeks of pregnancy.
What are contractions?
Contractions are the periodic tightening and relaxing of the uterine muscles. They are a crucial part of the labor process.
What is the difference between true labor and false labor?
True labor is characterized by regular contractions that become stronger, longer, and closer together over time. False labor, also known as Braxton Hicks contractions, are irregular and usually stop when you change positions or take a rest.
What is the active phase of labor?
The active phase of labor is the stage when the cervix dilates from 6 to 10 centimeters. During this stage, contractions become more intense and frequent.
How long does labor usually last?
The duration of labor can vary, but for most women, it lasts between 8 to 18 hours.
What can be done to induce labor?
If labor is not starting naturally or there are medical indications, healthcare providers may use various techniques to induce labor, such as using medication or performing artificial rupture of membranes.
What is a c-section delivery?
A C-Section delivery, also known as a cesarean delivery, is a surgical procedure in which the baby is delivered through an incision made in the mother’s abdomen and uterus.





